Contact Kulzer North America
-
Phone
(800) 431-1785

Gluma® Desensitizer
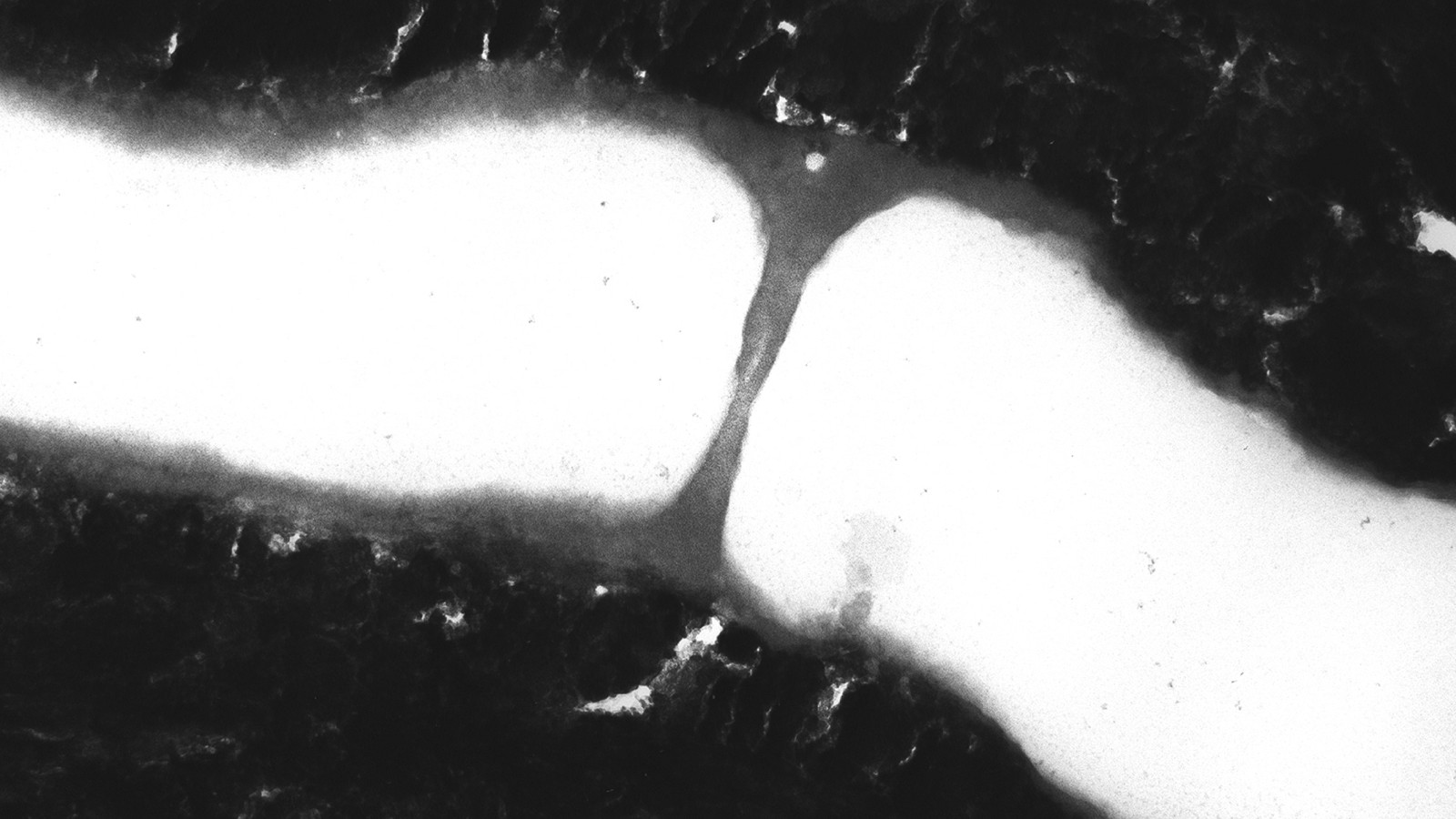
For over 20 years, one drop of Gluma® has been sufficient to reduce and prevent hypersensitivity. The results appear quickly and effectively, without mixing, curing or multiple applications. Your patients feel immediate relief.
Every good restoration starts with the Gluma® Desensitizer. Its efficacy has been proven in over 50 million restorations.
Benefits
Gluma® Desensitizer can be used under every restoration – direct and indirect – to ensure your patients the comfort they deserve.
- One-step Placement: No agitation or light curing required makes it easy to use and saves time.
- Universally Compatible: Gluma® Desensitizer can be used with bonding and restorative materials, in any situation.
- Economical: One drop, multiple applications.
Indications
For the reduction of hypersensitivity in exposed cervical areas and on teeth prepared to receive a restoration or a fixed prosthesis.
Applications
Step-by-step application
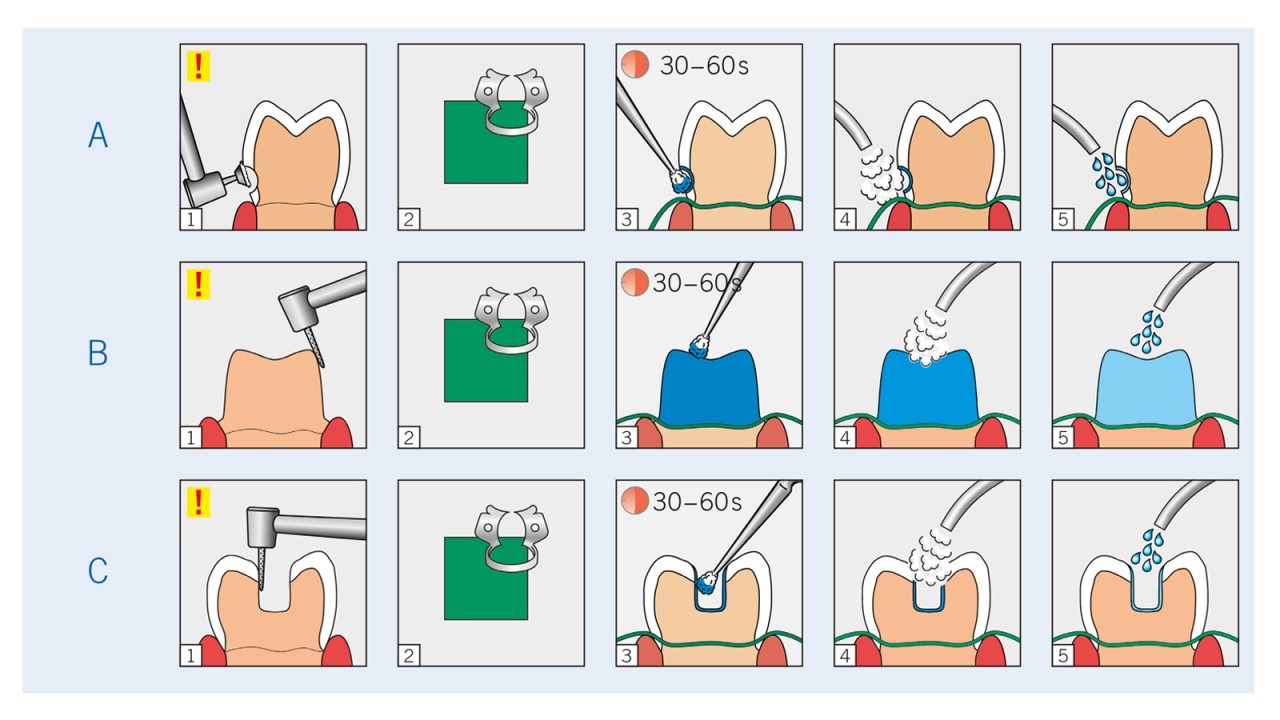
Science
Downloads
Contact
FIND YOUR SALES REP

No matches could be found. Please try again.
Please enter a valid zip code!
{{ targetGroup.name }}
{{ result.iosSpecialist }}
{{ result.zip }} {{ result.city }}
{{ result.fax }}